Here you can view summaries of our research projects, as well as affiliated collaboration projects relating to our work. For more in-depth information and links, head to our Outcomes & Engagements page.
Vinegar and Honey
The mixture of vinegar and honey, also known as Oxymel, has been used to treat a variety of immune system problems such as respiratory issues and coughing throughout many hundreds of years of human history. Honey is still used today to treat infections, but this use of a complex, raw natural product mixture is unusual in modern western medicine. Dr Freya Harrison, Dr Erin Connelly and their team at the University of Warwick conducted a systematic review to investigate published evidence for antimicrobial effects of vinegars against human pathogenic bacteria and fungi.
They then characterized selected vinegars by HPLC and assessed the antibacterial and antibiofilm activity of the vinegars
and acetic acid, alone and in combination with medical-grade honeys, against Pseudomonas aeruginosa and Staphylococcus
aureus. They found that some vinegars have antibacterial activity that exceeds that predicted by their acetic acid content alone,
but that this depends on the bacterial species being investigated and the growth conditions (media type, planktonic vs. biofilm). They also concluded that there is potential for
acetic acid, and some vinegars, to show synergistic antibiofilm activity with manuka honey.
Click the link above to view the conference poster for the project. Access to the full publication is available on our ‘Outcomes and Publications’ page.
'Bald's Eyesalve'

Our interdisciplinary team identified and reconstructed a potential remedy for Staphylococcus aureus (a bacterial skin infection). This remedy came from a 10th-century medical manuscript from Early Medieval England a.k.a a ‘leechbook’ (hence ‘Bald’s Leechbook’). The remedy repeatedly killed established S. aureus biofilms in an in vitro model of soft tissue infection and also killed methicillin-resistant S. aureus (MRSA) in a mouse chronic wound model. While the remedy contained several ingredients that are individually known to have some antibacterial activity, full efficacy required the combined action of several ingredients, highlighting the scholarship of pre-modern doctors and the potential of ancient texts as a source of new antimicrobial agents.
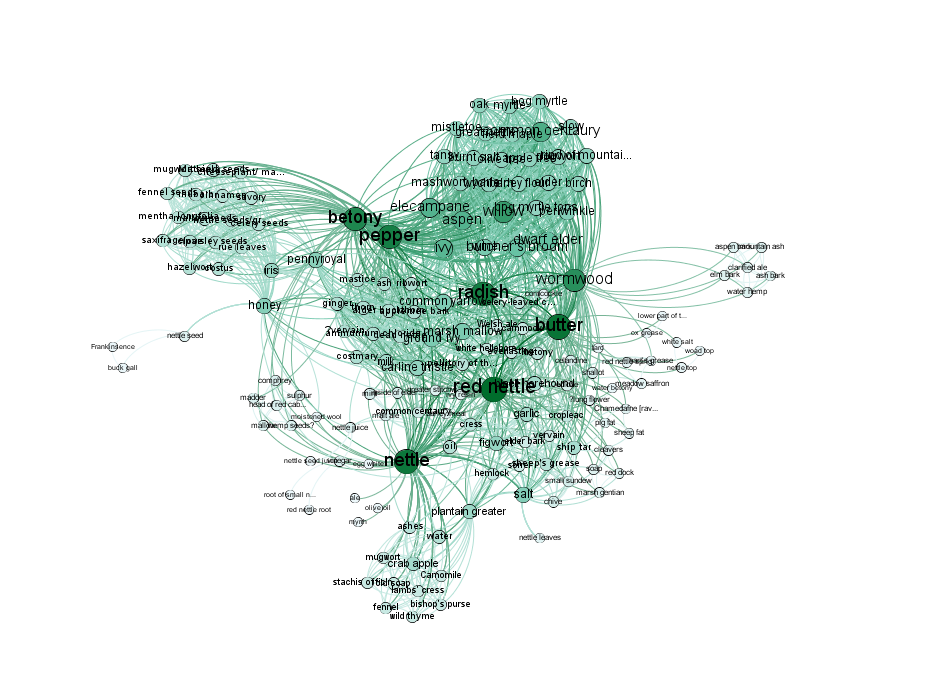
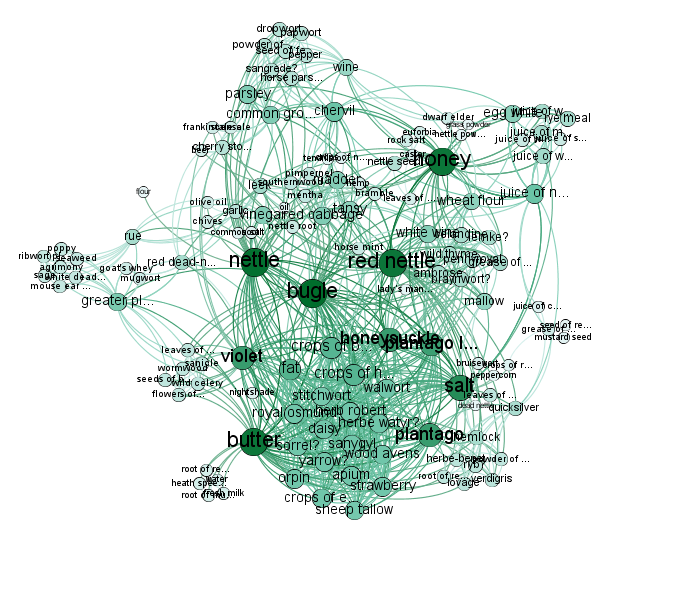
Nettles and Networks
Stinging nettles (Urtica spp.) have been used in a diverse range of traditional and historical medicines from around the world for the treatment of skin diseases, wounds, urinary disorders, respiratory diseases, bone and joint pain, anaemia and other circulatory problems, as well as in cosmetic preparations for skin and haircare. As part of an interdisciplinary exploration of nettle-based remedies, we performed a systematic review of published evidence for the antimicrobial activity of Urtica spp. extracts against bacteria and fungi that commonly cause skin, soft tissue and respiratory infections.
Our project examined if a combination of common ingredients shows antimicrobial activity. Our systematic review and additional experimental data leads us to conclude that there is no strong evidence for nettles containing molecules with clinically useful antimicrobial activity. It seems most likely that the utility of nettles in traditional topical preparations for wounds may simply be as a “safe” absorbent medium for keeping antibacterial (vinegar) or emollient (oils) ingredients at the treatment site.
Clinical translation of 'Bald’s Eyesalve'
We were awarded funding from Diabetes UK to explore whether Bald’s eyesalve has the potential to be developed into a natural product formulation that could be used to prevent and treat antibiotic-resistance biofilm infections of diabetic foot ulcers. These infections seriously impact quality of life for people with diabetes, and carry the risk of amputation or death from sepsis.
In this project, we showed that Bald’s eyesalve could kill biofilms of several bacterial species involved in diabetic ulcer infections – not just S. aureus. We also worked with new team members to conduct a detailed exploration of the likely safety of Bald’s eyesalve when applied to skin: this involved looking at its effects on human cells, in an animal model of a skin wound and – eventually – on the skin of healthy volunteers who wore a patch infused with the eyesalve for two days.
Finally, this project also allowed us to start dissecting the chemical composition of Bald’s eyesalve. We confirmed that its biofilm-killing ability requires more than one natural compound present in the original mixture, and were able to begin to design semi-synthetic derivatives of the eyesalve for future translational research.
Student Projects
Our first pilot work on treating wound pathogens with “ancientbiotics” made from nettles (Urtica species) was conducted by Navneet Jandu, an undergraduate student at the University of Warwick. This was a summer research project made possible by a Harry Smith Vacation Studentship from the Microbiology Society. Navneet’s results were built on by another Warwick undergraduate, Kate Willett, in a summer project funded by the University’s Undergraduate Research Support Scheme and supervised by Warwick PhD student Jessica Furner-Pardoe.

The Forschergruppe Klostermedizin



The Forschergruppe Klostermedizin (Allgemeines zur Forschergruppe, Research Group Monastic Medicine) was founded at the Institute for the History of Medicine at the University of Würzburg in 1999. It is a pharmaceutical-historical continuation of the “Würzburg Research Group” around Prof. Kurt Ruh, dealing with German prose from the Middle Ages since 1973 and also specifically with medical prose since the 1980s. The aim of the interdisciplinary project was initially to identify the medicinal plants used in the Middle Ages – especially in monastic medicine – and their applications in order to open up possibilities for modern research. For this purpose, some central works were edited and translated for the first time and individual plants and works were analyzed in the context of dissertations.
The scientific coordinator in the first 20 years was the philologist Dr. Johannes Gottfried Mayer († 2019), another important member was the pharmacist and biologist Prof. Franz-Christian Czygan († 2012). Right from the start, the team has included physician and physicist Prof. Bernhard Uehleke and pharmacist Katharina Mantel. The current coordinator, Dr. Tobias Niedenthal, has been a member of the group since 2010, the biologist Dr Elke Puchtler joined 2019.
The research group is now dealing with the entire history of medicinal plants in the extended European cultural area (including North Africa and the Middle East), with a focus on the historical and modern use of herbal antimicrobials. Since its foundation, the research group has been in the media regularly and strives to offer interested laypeople scientifically sound access to the medicine of the Middle Ages and modern phytotherapy.
For more information see: Tobias Niedenthal and Forschergruppe Klostermedizin.
Images via http://www.klostermedizin.de/





